A Year In Vaccines: How The UK Become A World-Leader In Mass Vaccination
11 min read
On 8 December 2020, 90-year-old grandmother Margaret Keenan became the first person in the world to receive a Pfizer Covid-19 vaccine outside clinical trials. Since then, over 47 million people — around 82% of the UK population — have had two vaccine doses.
The sheer scale of Britain’s remarkable vaccine rollout is something that would have seemed impossible just a few years ago.
And it’s far from over. Now, the country is entering the next stage of this journey as the government calls on all adults to get a booster jab to fend off the new Omicron variant.
Here’s a look back at how the UK became a world-leader in mass vaccination:
MARCH - DECEMBER 2020
Sporting a festive penguin jumper, Margaret Keenan’s historic jab marked the end of the first stage of the government’s vaccine rollout. Much of the work to get needles in arms started many months earlier, just as the country was plunged into its first lockdown.
The government launched its Vaccine Taskforce on 17 April 2020 with the set aim of expediting the approval process for vaccines and helping the UK secure the millions of doses needed.
By July, the UK had already bought up 90 million doses of AstraZeneca and Pfizer’s products, despite the fact there was no evidence either actually worked.
Luckily, this expensive gamble paid off. Evidence from Phase III trials of the Pfizer/BioNTech, published in November, suggested that it was 95% effective in preventing severe cases of Covid-19. Within days of that data, the UK became the first country in the world to approve the Pfizer vaccine on 2 December. Six days later, Keenan got her jab. Under Phase One of the vaccine rollout, the most vulnerable would get their jab first, starting with care home residents, their carers, and adults aged 80 and over. By Christmas Eve, 600,000 people had received their first dose.
Within days of that data, the UK became the first country in the world to approve the Pfizer vaccine on 2 December. Six days later, Keenan got her jab. Under Phase One of the vaccine rollout, the most vulnerable would get their jab first, starting with care home residents, their carers, and adults aged 80 and over. By Christmas Eve, 600,000 people had received their first dose.
Starting procurement and vaccination so quickly — much faster than our European counterparts — was a “great lesson” of the rollout, according to JCVI deputy chair Dr Anthony Harnden.
“We accelerated the vaccines through the regulatory system, which was excellent,” he told PoliticsHome.
“So we were able to get them much earlier than you would possibly imagine, and the vaccines turned out to be hugely more effective than we ever thought.”
Just as the Oxford/AstraZeneca jab was approved, on 30 December, the government also increased the waiting period between vaccine doses from three to 12 weeks to speed up the rollout.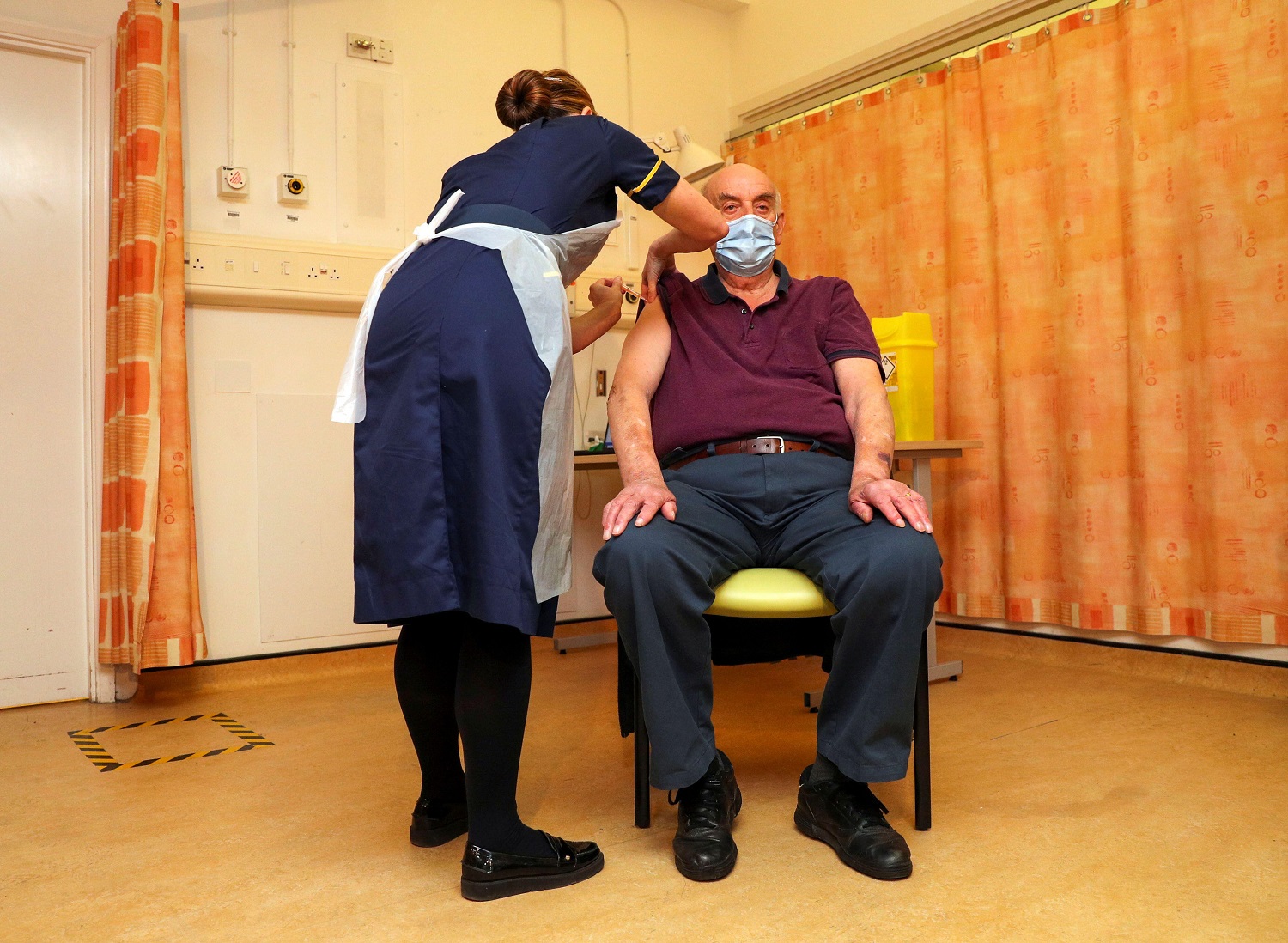
JANUARY 2021
A lot happened in the first 10 days of 2021. On 4 January, 82-year-old Brian Pinker became the first person outside trials to get an Oxford/AstraZeneca vaccine. Two days later, the country went into its third national lockdown. The UK then approved its third vaccine, the American-made Moderna jab, on 8 January. By 10 January, 1.5 million people had been given their first dose.
Ministers published a plan to get the nation immunised the following week, setting out an aim of administering at least 2 million vaccinations per week at over 2,700 vaccine sites across the UK. The next phase of the rollout was vaccinating those aged 70 and over and clinically extremely vulnerable individuals, which began on 18 January.
FEBRUARY
There were some teething problems early in the rollout. Ministers were forced to admit that they hadn’t hit their target of offering vaccines to all care home staff by the end of January, despite managing to jab all care home residents.
The UK did hit its first big vaccine milestone, however, on 3 February as 10 million people had now received their first vaccine dose. By mid-February, the rollout had been expanded to include everyone over 65, and anyone over 16 with severe underlying health conditions. The country was still in lockdown at the time, with the PM setting out the roadmap to lift restrictions on 22 February.
MARCH
Things kept on ramping up in March. Over 60s were offered their jab from 1 March, and then over 50s from 17 March. Midway through the month, the next milestone was hit — 25 million first doses.
Concerns had been raging across Europe for weeks over the safety of the AstraZeneca vaccine, amid fears it may be causing rare blood clots. But, the MHRA insisted the jab was safe. Boris Johnson reiterated this at a press conference, claiming the benefits of the jab "far outweigh the risks" and announcing he’d be getting his own dose of AstraZeneca that weekend.

APRIL
Despite being approved in January, supply constraints meant the first Moderna dose wasn’t administered until 7 April. It was given to 24-year-old Elle Taylor, an unpaid carer from Carmarthenshire.
One of the biggest changes to the rollout came a day later on 8 April. The government accepted advice from the Joint Committee on Vaccination and Immunisation (JCVI), the government recommended that under 30s shouldn’t be given the AstraZeneca vaccine amid ongoing concerns over blood clots.
The government officially entered Phase Two of its vaccination programme on 13 April, offering jabs to the adult population starting with those aged 45 and over.
MAY
The next big vaccine milestone was hit on 3 May, with 50 million first doses having been administered nationwide. Vaccines were now being offered to everyone aged 40 and over, and England was approaching its final stages of lockdown lifting.
Fresh advice from the JCVI meant that, from 7 May, those aged 30 to 39 without underlying health conditions would also be offered an alternative to the Oxford/AstraZeneca vaccine amid blood clot fears. This age group was also the next to be called for their first dose, working down through the 30s a year at a time, with appointments made available to the whole age group from 26 May.
On 28 May, the MHRA approved the country’s fourth vaccine — the dutch-made Janssen vaccine, which could be administered in a single dose.
JUNE
Just as the country approached its “freedom day” when most of the remaining lockdown restrictions would be scrapped, efforts to get needles in arms were ramped up once again.
By 3 June, three quarters of UK adults had been given one dose, and half were fully vaccinated. The call quickly went down the age brackets, with adults aged 25 and over eligible from 8 June, and those aged 21 and over from 16 June. By 18 June, everyone aged 18 and over could book their first dose.
According to Dr Harnden, it was the “simplicity” of the government’s phased approach that contributed to its success.
“We designed a programme that could be rolled out at speed, that was deliverable and was simple. People understood where they were in the queue order in terms of getting their vaccine, and that helped enormously in promoting uptake,” he said.
While the country reeled at the success of its rollout, the JCVI issued interim advice on the next phase — boosters. It proposed that the most vulnerable members of society should start being offered a third vaccine dose from September.
JULY
July brought the much-awaited “freedom day” in England, as well as the news that over two thirds of UK adults had been double vaccinated.
By 19 July, the day restrictions ended, everyone over 18 had been offered the chance to book both doses. The rollout was also expanded, following advice from the JCVI, to include vulnerable 12- to 15-year-olds.
By this point, over 128,000 people had died within 28 days of contracting coronavirus. But, as Dr Michael Head, Senior Research Fellow at the University of Southampton, reflects, it could have been so much worse.
“[It’s] quite the sobering thought, and given the burden of Covid-19 disease we still have, I shudder to think where we would be without the deployment of these vaccines.”
“The current UK and global situation does, however, show that while vaccines can do a fair amount of the heavy lifting, a better pandemic response cannot rely on vaccines alone.”
AUGUST
August began with the news that 16 and 17-year-olds would soon be called to get their first vaccine. The JCVI announced on 4 August that data suggested the Pfizer vaccine was safe for children aged over 12, but would be offered to older children first. A few weeks later, the Moderna vaccine was also approved by the MHRA for use on 12- to 17-year-olds.
Some questioned the wisdom of this decision, however, arguing that these doses would be better deployed elsewhere in the world.
“We have not done anywhere near enough to ensure vaccine equity across the world and that may have been one of the factors that enabled Omicron to evolve,” Dr Paul Hunter, professor in medicine at the University of East Anglia, told PoliticsHome.
“We chose to offer vaccines to our children despite JCVI saying that vaccination in teenagers had only marginal benefit when those vaccines could have done more good elsewhere in the world.”
SEPTEMBER
Plans for booster jabs were given the green light on 1 September, with all people aged 12 and over who have “severely suppressed immune systems” eligible. The JCVI later said that third jabs would also be offered to all over 50s and frontline health and social care staff during the winter period alongside the annual flu jab.
The vaccine rollout was also expanded again on 13 September to include all children aged 12 and over, following a recommendation from the UK's four Chief Medical Officers. For now, this age group was only being offered one jab, with details of the second to be decided at a later date.

OCTOBER
As of 1 October, 45 million people — 78% of the UK population — had been given two vaccine doses. Polling seen by PoliticsHome, however, suggested that less than half of 12- to 15-year-olds had been vaccinated, despite the age group being eligible for over a month.
The government’s focus quickly shifted towards winter, with numerous advertising campaigns published urging those eligible to get their booster vaccine alongside their flu jabs.
NOVEMBER
By 1 November, 8 million eligible people had been given their coronavirus booster jab. Two weeks later, the programme was extended to include everyone aged 40 and over, and those aged 16 and 17 were invited to get their second vaccine.
Meanwhile, a new variant of coronavirus — Omicron — was identified as a variant of concern by the World Health Organisation (WHO). Announcing its discovery on 26 November, the WHO said Omicron “has a large number of mutations, some of which are concerning” and that strain appeared to be much more transmissible than its predecessor Delta.
Just days later, on 29 November, the health secretary announced that the booster programme would be massively ramped up in response to this discovery. Javid said the move was to help Britain “buy the time we need” to assess how serious Omicron was.
The government promised to offer a booster jab to all UK adults by the end of January. To hit this target, the wait between the second and third dose was halved from six months to three, allowing many more people to come forward.
According to Dr Hunter, the speed of this response may prove key. “We are ahead of almost all countries on the roll out of the booster dose which, although we didn’t know it at the time, may be the thing that makes all the difference with the Omicron variant,” he told PoliticsHome.
DECEMBER
By 10 December, over 22 million top-up jabs had been delivered across the UK, meaning close to 40% of the adult population had now had three doses.
Boris Johnson announced on 12 December that he hoped to soon be administering 1 million jabs a day as part of the rollout — significantly higher than the record 844,000 delivered in a single day in March.
On 18 December, the target of 1million booster doses in a day was hit for the first time in the UK.
On 22 December, the MHRA recommended that vulnerable children aged five-11 should be offered a Covid vaccine. A decision by the Chief Medical Officer on whether to approve the roll-out is expected soon.
Calls remain, however, for the UK to do more to support the global vaccination effort, rather than focus solely on immunising its own population.
“As we see with Omicron likely emerging from southern Africa, and previously the Delta variant in India – variants are more likely to emerge from uncontrolled outbreaks,” said Dr Head.
“Where populations are more highly vaccinated, the lower those risks. This particular novel coronavirus simply has not finished with us yet, and an urgent global cooperation around the distribution of vaccines is vital.”
