Doctors Warn NHS Could Be “Dead In The Water” If Summer Surge Increases A&E Demand
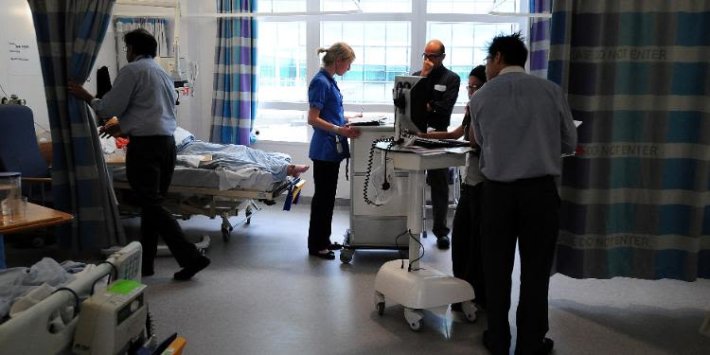
"The profession was stretched before Covid-19, but the pandemic has exacerbated this.” (Alamy)
4 min read
Medical professionals have warned that a surge in coronavirus cases could overwhelm the NHS as the health service continues to battle with coronavirus alongside a return to pre-pandemic demand.
Analysis of NHS data by PoliticsHome reveals that around 52,000 additional people visited emergency departments in England last month when compared to pre-pandemic figures from June 2019 — a 2.4% increase overall.
Meanwhile, A&E attendance and admissions figures have increased in every region of England as the country lifts remaining lockdown restrictions, with June seeing the highest numbers since records began.
Doctors are concerned that this uptick in people attending A&E could prove unmanageable if it coincides with the surge in coronavirus cases expected in the coming months.
“In the previous waves, what we've seen is that as soon as Covid kicks off, a lot of the other patients seem to stay away,” one A&E consultant told PoliticsHome.
“If the same happens this time we might get away with it, but if the demand we've currently got doesn't ease up, and we get decent numbers of Covid on top of it, then we are just going to be absolutely dead in the water.”
Health secretary Sajid Javid has warned that the UK could face a daily infection rate of 100,000 by mid-Summer, with Sage modelling suggesting the peak of the next wave could hit at the end of August.
Javid suggested that the effects of the vaccine rollout would mean hospitalisations and deaths would not rise in line with cases.
But Adrian Boyle, vice president of the Royal College of Emergency Medicine, said even a small number of additional coronavirus admissions could be “very disruptive” to the already-stretched service, describing the virus as “one heavy straw on the camel’s back”.
“We are in a position now of really, really increased demand, but this is not related to Covid. It is not because of lots of Covid cases coming into our hospitals,” he said, speaking to PoliticsHome.
“The demand level in terms of number of patients has probably gone up in line with what we would expect.”
“The difference is that the hospitals have lost beds because of all the necessary infection prevention and control measures.”
“We've lost about 6,000 beds as a consequence of all the necessary things we need to do to maintain social distance within hospitals.”
Alongside a record increase in attendances, June also saw the lowest number of people treated within 4 hours of arrival on record at 73.2%. Around 1,289 people were also subjected to 12-hour plus waits to be admitted – almost double the number for May 2021.
“For the last couple of months, what we've been seeing is a lot more walk-in patients — particularly children,” an A&E doctor told PoliticsHome.
“We usually get big numbers of walk-ins over the summer and during the school holidays. Whereas for the last two months, during term time as well, we've just been getting lots of adults and children coming in with relatively minor stuff.”
“Some of it certainly seems to be around access to GPs, as far as I can tell the GPs themselves are swamped… think what's happening at the moment is the parents can't get appointments.
“And then they're getting through to 111 and they tend to play it safe and send them to us. Likewise, when they're getting through to the GPs on the phone, they’re often doing a phone assessment and decide the safe thing to do is to send the kid up to us.”  Professor Martin Marshall, Chair of the Royal College of GPs, agreed about the pressures facing primary care providers.
Professor Martin Marshall, Chair of the Royal College of GPs, agreed about the pressures facing primary care providers.
He said: “GPs and our teams are currently working under intense pressure, making record numbers of patient consultations — more than 22m in the four weeks up to 27 June — alongside delivering around two thirds of the Covid vaccination programme.
“This increasing workload, both in terms of volume and complexity, is against a backdrop of falling GP numbers. The profession was stretched before Covid-19, but the pandemic has exacerbated this.”
But he dismissed suggestions that doctors were sending patients to A&E needlessly, claiming “GPs will only recommend patients attend A&E if they think it’s the most appropriate place for them to go to get the care they need.”
He continued: “In general practice, we simply don’t have enough GPs or other members of the practice team to meet demand and we’re only set to get busier as we continue to support our communities’ recovery from the pandemic, and approach what is set to be a very difficult winter.”
The Department for Health and Social Care declined to comment. NHS England pointed to a reduction in the number of people waiting 18-52 weeks waiting to begin non-urgent treatment despite record numbers of people attending A&E in June.
